Volume: 18 Issue: 6 November 2020
FULL TEXT
Objectives: Our aim was to investigate effects of surgery on living donors’ body composition and clarify factors related to it.
Materials and Methods: We evaluated preoperative computed tomography images of 335 living kidney donors (127 men, 209 women) to calculate 3 body composition parameters and changes with aging by sex: (1) skeletal muscle mass, quantified by skeletal muscle index; (2) fat distribution, calculated by visceral adipose tissue/subcutaneous adipose tissue ratio; and (3) muscle quality, quantified by intramuscular adipose tissue content. Thereafter, with pre- and postoperative computed tomography images from 75 living kidney donors (25 men, 50 women) after hand-assisted laparoscopic donor nephrectomy, we compared pre- and postoperative body composition changes.
Results: Annual change in intramuscular adipose tissue content with age was 0.0049 in men and 0.0091 in women. Of 75 patients, 49 had lower quality of muscle, intramuscular adipose tissue content was significantly higher after nephrectomy (P < .001), and median change in intramuscular adipose tissue content was 0.061 (range, 0.018-0.11) in men and 0.052 (range, 0.017-0.18) in women. Univariate analysis revealed that skeletal mass index and visceral adipose tissue/subcutaneous adipose tissue ratio changes were significantly different between the intramuscular adipose tissue content improvement and deterioration groups. Multivariate analysis revealed skeletal mass index change was an independent factor for intramuscular adipose tissue content change (P = .0019). Intramuscular adipose tissue content change was negatively correlated with skeletal mass index change (r = -0.40).
Conclusions: Although muscle quality deteriorates after nephrectomy, maintaining muscle mass is important to retaining muscle quality.
Key words : Intramuscular adipose tissue content, Skeletal muscle index, Subcutaneous adipose tissue, Visceral adipose tissue
Introduction
Living donor nephrectomy is a major burden on living donors because of surgical stress and the possibility of inducing chronic postsurgical pain.1-3 Minimally invasive surgery such as laparoscopic donor nephrectomy (LDN) is one way to reduce this burden because of its reduced invasiveness, less postoperative pain, shorter duration of stay, and earlier return to normal physical activity and work compared with open donor nephrectomy.4-6 The safety and minimal complications of LDN are also well recognized, but few reports are available on the effects of LDN on body composition, which is greatly affected by surgery.
Body composition represents the relative proportion of fat, bone, and muscles in our body. The quantification of muscle and adipose tissue, known as body composition analysis, is widely used in various fields as an indicator of patient health.7 Muscle mass and muscle quality are the most well-known parameters in body composition analysis and are related to sarcopenia.8,9 Fat distribution is another widely recognized parameter and is related to cardiovascular disease.10 Body composition analysis is also important in surgical fields, as the results can be associated with outcomes such as risks during the postoperative course and graft survival.11-14 Preoperative and postoperative body composition analyses are important to predict the postoperative course and to check the health of living donors preoperatively and postoperatively.
Although several modalities are available to assess body composition, computed tomography (CT) is considered optimal to measure muscle mass, muscle quality, and fat distribution in clinical settings. Moreover, CT is often performed for surgical planning to understand the courses and numbers of blood vessels or to identify structures such as the ureter in the kidney.
The aim of this study was to evaluate and compare body composition (muscle mass, muscle quality, and fat distribution) before surgery and 1 year after living donor nephrectomy and to investigate factors related to body composition changes.
Materials and Methods
Patient selection
This study was retrospective, and the analysis used anonymous clinical data. Thus, the need for informed consent was waived for this study (approval no. 1382S).
To investigate sex-specific and age-related changes in muscle mass, muscle quality, and body fat distribution, the medical records of 336 living kidney donors (127 men, 209 women) who underwent hand-assisted laparoscopic living donor nephrectomy (HALDN) from April 2015 to March 2018 in our institution were retrospectively reviewed. Of the 336 patients, 1 man was excluded because the CT images could not be analyzed by the CT analysis software. Thus, 335 patients were included in this retrospective study. The patients’ median age was 64 years (range, 34-76 years) in men and 59 years (range, 32-76 years) in women. Regarding the type of donor, spousal donor was the most common (n = 175; 52.2%), followed by first-degree related donor (n = 121; 36.1%), second-degree related donor (n = 38; 11.3%), and third-degree related donor (n = 1; 0.3%).
To compare body composition between before surgery and 1 year after HALDN, the medical records of 201 patients who underwent HALDN in our institution between April 2016 and March 2018 were reviewed. Of these, 136 patients who were followed-up at another institution were excluded. Thus, 75 patients were included in this retrospective comparative analysis. Regarding type of donor, first-degree related donor was the most common (n = 38; 50.7%), followed by spousal donor (n = 28; 37.3%), and second-degree related donor (n = 9; 12.0%).
Imaging analysis
Skeletal muscle and adipose tissue were analyzed to calculate 3 body composition indexes: skeletal muscle index (SMI), intramuscular adipose tissue content (IMAC), and ratio of visceral adipose tissue (VAT) to subcutaneous adipose tissue (SAT). These indexes were determined from preoperative cross-sectional plain CT images processed with AZE Virtual Place automated planimetry software (AZE Ltd., Tokyo, Japan) on a dedicated offline workstation. All CT studies were performed with a multidetector-row helical CT scanner using a tube voltage of 120 kV and a reconstruction slice thickness of 5 mm.
The SMI was calculated using the skeletal muscle area at the L3 level assessed by manual tracing with AZE Virtual Place software (Figure 1A), where SMI is the cross-sectional area of all skeletal muscle in centimeters squared divided by the height in meters squared. The skeletal muscles at the L3 level were as follows: rectus abdominis muscle, external oblique muscle, internal oblique muscle, transversus abdominis muscle, psoas major muscle, quadratus lumborum muscle, erector spinae muscle, latissimus dorsi muscle, and multifidus lumborum muscle (Figure 1A). The IMAC value represents muscle quality. Higher IMAC values indicate greater deterioration of muscle quality. The IMAC value was calculated with L3-level CT cross-sectional images, with IMAC equal to the mean CT attenuation value (measured in Hounsfield units [HU]) in the region of interest of multifidus muscle divided by the mean CT attenuation value in the region of interest of subcutaneous fat (Figure 1B). The VAT-to-SAT ratio (VAT/SAT) was also calculated with cross-sectional umbilical-level CT images (Figure 1C). Subcutaneous adipose tissue was defined as the extraperitoneal fat between skin and muscles with CT attenuation values within the range from -190 to -50 HU on 1 of the constructed images. Visceral adipose tissue was defined by intraperitoneal fat with the same density as the SAT layer. Segmentation of abdominal SAT and VAT areas was determined using AZE Virtual Place software. Higher values indicate lower quality fat distribution.
Statistical analyses
In the sex-specific and age-related analysis of body composition changes, the Shapiro-Wilks normality test was used to assess the normality of the distributions of continuous data. Correlations between continuous variables were assessed with the Pearson correlation coefficient for normally distributed data and with the Spearman rank correlation coefficient for other data. With linear coefficients, age-adjusted values for SMI, IMAC, and VAT/SAT were calculated.
In the retrospective comparative analysis, preoperative and postoperative body composition parameters (SMI, IMAC, VAT, SAT, and VAT/SAT) and body mass index (BMI, calculated as weight in kilograms divided by height in meters squared) were compared with the t test or the Mann-Whitney U test. Among these body composition parameters, those with significant changes were then divided into the improvement and deterioration groups.
When the 2 groups were compared, the chi-square test or the Fisher exact test was used for categorical variables, and the t test or Mann-Whitney U test was used for continuous variables. Logistic regression analysis was used for significant variables on multivariate analysis, and then the odds ratios (OR), P values, and 95% confidence intervals were calculated. Receiver operating characteristic curve analysis and the area under the curve were used to determine body composition changes. P < .05 was considered significant. All analyses were performed with EZR software (Saitama Medical Center, Jichi Medical University, Saitama, Japan).
Results
Evaluations of skeletal muscle index, intramuscular adipose tissue content, and subcutaneous versus visceral adipose tissue
Using preoperative CT images from 335 patients, we analyzed SMI, IMAC, and VAT/SAT. There was a significant negative relationship between SMI and age in both men and women. The annual change in SMI with age was -0.18 in men and -0.21 in women. There was a significant positive relationship between IMAC and age in both men and women. The annual change with age was +0.0049 in men and +0.0091 in women. There was a significant positive relationship between VAT/SAT and age in both men and women. The annual change with age was +0.0149 in men and +0.0082 in women.
Body composition comparison
Using the preoperative and postoperative CT images of 75 patients, a comparative analysis of body composition was performed. Table 1 shows the comparisons of 6 body composition parameters (SMI, IMAC, VAT, SAT, VAT/SAT, and BMI) between before surgery and 1 year after surgery, showing that IMAC was significantly more deteriorated postoperatively versus preoperatively.
Intramuscular adipose tissue content analysis
The 75 patients were divided into IMAC improvement and deterioration groups. Figure 2 shows that, of the 75 patients, 49 patients (65.3%; 16 men, 33 women) demonstrated deteriorated muscle quality. For these 49 patients, median change in IMAC
was 0.061 (range, 0.018-0.11) in men and 0.052
(range, 0.017-0.18) in women. Table 2 shows the characteristics of patients in these 2 subgroups before and after surgery. There was no significant difference in background factors between the 2 groups except for a history of diabetes mellitus and preoperative hemoglobin level. Table 3 shows the univariate and multivariate analyses of changes in renal function and body composition from before surgery to 1 year after surgery between the IMAC improvement and deterioration groups. The SMI change and VAT/SAT change in the 2 groups were significant on univariate analysis. Logistic regression demonstrated that SMI change could be a significant factor for IMAC change. Figure 3A shows correlation data between IMAC change and SMI change, showing a moderate negative correlation (r = -0.40). Receiver operating characteristic curve analysis showed an area under the curve value of 0.79 (95% confidence interval,
0.68-0.90) for SMI change from before surgery to 1 year after surgery as a predictor of IMAC change (Figure 3B). A cutoff value for SMI change of 0.68 predicted patients with IMAC improvement 1 year after surgery with sensitivity of 0.71 and specificity of 0.83.
Discussion
This study provided 2 useful clinical observations. First, among the body composition parameters examined, IMAC was the most affected after donor nephrectomy. Effects of surgery on muscle mass or fat mass have been described in many papers,15-18 but reports on IMAC are few. Intramuscular adipose tissue content is closely related to sarcopenia, which provides a barometer of patient health and is associated with physical performance, risk of falls, and fracture risk.8,19-21 Assessment of IMAC is therefore important when considering donor health postoperatively.
Second, IMAC change was associated with SMI change. There have been several studies showing the relationships between IMAC and SMI. Fukuda and colleagues reported a negative relationship between IMAC and skeletal muscle mass (r = -0.51) among recipients of pancreatic tiontion.11 Matsubara and colleagues reported that IMAC deterioration was strongly correlated with skeletal muscle wasting (r = 0.70).8 Moreover, both IMAC and SMI are related to sarcopenia. Maintaining muscle mass therefore not only helps prevent sarcopenia, but also helps prevent IMAC deterioration.
Numerous studies have reported the effectiveness of exercise in preventing sarcopenia. For example, Shephard and colleagues reported that the risk of developing sarcopenia was substantially lower among elderly people taking at least 7000 to 8000 steps per day or exercising for at least 15 to 20 minutes per day at an intensity greater than 3 metabolic equivalents.22 Akune and colleagues reported that achieving sweating or shortness of breath during exercise (occasionally or about 2 hours each week) in middle age (25-50 years old) was associated with less sarcopenia in older patients and was effective in maintaining muscle strength and physical performance in older patients.23
Nutrition was another key factor in maintaining or improving skeletal muscle mass. Muscariello and colleagues reported that protein intake of 1.2 g/kg desirable body weight per day in addition to a caloric intake of approximately 20 to 25 kcal/kg desirable body weight per day was effective in preserving muscle mass in sarcopenic obese older women.24 Yang and colleagues reported that a diet containing meat, egg, and milk 4 to 7 times a week helped prevent sarcopenia.25
Although prospective cohort studies are needed to develop an IMAC maintenance program, moderate exercise and a diet with high protein have been found to be important factors for maintaining IMAC.
There were several limitations to this research. First, preoperative and postoperative lifestyle factors, such as smoking, eating habits, and frequency of consuming alcohol, which all affect body composition, were not considered in the present investigation.26-28 In this study, differences in history of diabetes mellitus and preoperative hemoglobin level were seen between IMAC improvement and IMAC deterioration groups. Patients in IMAC improvement group showed higher hemoglobin level and a greater frequency of a history of diabetes mellitus. These patients may be in the habit of eating greater proportions of iron- and protein-rich foods such as fish, meat, egg, and soy foods, which are useful for maintaining muscle mass. Moreover, living kidney donors with diabetes mellitus may be more conscientious about preoperative and postoperative diet. Of the 49 patients whose IMAC deteriorated in the present study, 19 patients (38.8%) had increased SMI. Analysis of lifestyle will help determine the reasons for IMAC deterioration in the 19 patients who maintained their SMI.
Second, only patients who underwent HALDN were investigated. Therefore, whether the present results are applicable to other surgical methods, such as open nephrectomy or pure laparoscopic nephrectomy, remains unclear. However, HALDN, but also pure laparoscopic surgery or open surgery, will likely still affect body composition. Choi and colleagues compared body composition changes in mucosal gastric cancer patients in those who had laparoscopic surgery versus open surgery. They concluded that both surgical techniques affected body composition but that body composition changes were likely less with laparoscopic surgery than with open surgery.29
Conclusions
Although muscle quality deteriorates after HALDN, maintaining muscle mass is significantly associated with retaining muscle quality. To maintain donor health, a muscle rehabilitation program including an exercise regimen should be recommended to donors after nephrectomy. Moreover, living kidney donors should receive explanations about the importance of postoperative exercise before donor nephrectomy.
References:
- Bahler CD, Sundaram CP. Quality of life following laparoscopic living-donor nephrectomy. JSLS. 2013;17(2):273-278. doi:10.4293/10860813X13693422521395
CrossRef - PubMed - Rodrigue JR, Schold JD, Morrissey P, et al. Mood, body image, fear of kidney failure, life satisfaction, and decisional stability following living kidney donation: Findings from the KDOC study. Am J Transplant. 2018;18(6):1397-1407. doi:10.1111/ajt.14618
CrossRef - PubMed - Bruintjes MHD, van Helden EV, de Vries M, et al. Chronic pain following laparoscopic living-donor nephrectomy: prevalence and impact on quality of life. Am J Transplant. 2019;19(10):2825-2832. doi:10.1111/ajt.15350
CrossRef - PubMed - El-Galley R, Hood N, Young CJ, Deierhoi M, Urban DA. Donor nephrectomy: a comparison of techniques and results of open, hand assisted and full laparoscopic nephrectomy. J Urol. 2004;171(1):40-43. doi:10.1097/01.ju.0000100149.76079.89
CrossRef - PubMed - Mansour AM, El-Nahas AR, Ali-El-Dein B, et al. Enhanced recovery open vs laparoscopic left donor nephrectomy: a randomized controlled trial. Urology. 2017;110:98-103. doi:10.1016/j.urology.2017.08.047
CrossRef - PubMed - Tsuchiya N, Satoh S, Sato K, et al. Hand assisted retroperitoneoscopic living donor nephrectomy in elderly donors. J Urol. 2006;175(1):230-234; discussion 234. doi:10.1016/S0022-5347(05)00043-1
CrossRef - PubMed - Troschel AS, Troschel FM, Best TD, et al. Computed tomography-based body composition analysis and its role in lung cancer care. J Thorac Imaging. 2020;35(2):91-100. doi:10.1097/RTI.0000000000000428
CrossRef - PubMed - Matsubara Y, Furuyama T, Nakayama K, et al. High intramuscular adipose tissue content as a precondition of sarcopenia in patients with aortic aneurysm. Surg Today. 2018;48(12):1052-1059. doi:10.1007/s00595-018-1697-9
CrossRef - PubMed - Bahat G, Tufan A, Tufan F, et al. Cut-off points to identify sarcopenia according to European Working Group on Sarcopenia in Older People (EWGSOP) definition. Clin Nutr. 2016;35(6):1557-1563. doi:10.1016/j.clnu.2016.02.002
CrossRef - PubMed - Kunimura A, Ishii H, Uetani T, et al. Impact of adipose tissue composition on cardiovascular risk assessment in patients with stable coronary artery disease. Atherosclerosis. 2016;251:206-212. doi:10.1016/j.atherosclerosis.2016.06.041
CrossRef - PubMed - Fukuda Y, Asaoka T, Eguchi H, et al. Clinical impact of preoperative sarcopenia on the postoperative outcomes after pancreas transplantation. World J Surg. 2018;42(10):3364-3371. doi:10.1007/s00268-018-4639-1
CrossRef - PubMed - Hamaguchi Y, Kaido T, Okumura S, et al. Proposal for new selection criteria considering pre-transplant muscularity and visceral adiposity in living donor liver transplantation. J Cachexia Sarcopenia Muscle. 2018;9(2):246-254. doi:10.1002/jcsm.12276
CrossRef - PubMed - Noguchi H, Miyasaka Y, Kaku K, et al. Preoperative muscle volume predicts graft survival after pancreas transplantation: a retrospective observational cohort study. Transplant Proc. 2018;50(5):1482-1488. doi:10.1016/j.transproceed.2018.03.018
CrossRef - PubMed - van Dijk DP, Bakens MJ, Coolsen MM, et al. Low skeletal muscle radiation attenuation and visceral adiposity are associated with overall survival and surgical site infections in patients with pancreatic cancer. J Cachexia Sarcopenia Muscle. 2017;8(2):317-326. doi:10.1002/jcsm.12155
CrossRef - PubMed - Hopkins JJ, Reif R, Bigam D, Baracos VE, Eurich DT, Sawyer MM. Change in skeletal muscle following resection of stage I-III colorectal cancer is predictive of poor survival: a cohort study. World J Surg. 2019;43(10):2518-2526. doi:10.1007/s00268-019-05054-3
CrossRef - PubMed - Lee SJ, Kim JY, Ha TK, Choi YY. Changes in lipid indices and body composition one year after laparoscopic gastrectomy: a prospective study. Lipids Health Dis. 2018;17(1):113. doi:10.1186/s12944-018-0729-1
CrossRef - PubMed - Lee YH, Han SJ, Kim HC, et al. Gastrectomy for early gastric cancer is associated with decreased cardiovascular mortality in association with postsurgical metabolic changes. Ann Surg Oncol. 2013;20(4):1250-1257. doi:10.1245/s10434-012-2688-5
CrossRef - PubMed - Maimoun L, Lefebvre P, Aouinti S, et al. Acute and longer-term body composition changes after bariatric surgery. Surg Obes Relat Dis. 2019;15(11):1965-1973. doi:10.1016/j.soard.2019.07.006
CrossRef - PubMed - Yu R, Leung J, Woo J. Sarcopenia combined with FRAX probabilities improves fracture risk prediction in older Chinese men. J Am Med Dir Assoc. 2014;15(12):918-923. doi:10.1016/j.jamda.2014.07.011
CrossRef - PubMed - Beaudart C, Reginster JY, Petermans J, et al. Quality of life and physical components linked to sarcopenia: The SarcoPhAge study. Exp Gerontol. 2015;69:103-110. doi:10.1016/j.exger.2015.05.003
CrossRef - PubMed - Spira D, Buchmann N, Nikolov J, et al. Association of low lean mass with frailty and physical performance: a comparison between two operational definitions of sarcopenia. Data from the Berlin Aging Study II (BASE-II). J Gerontol A Biol Sci Med Sci. 2015;70(6):779-784. doi:10.1093/gerona/glu246
CrossRef - PubMed - Shephard RJ, Park H, Park S, Aoyagi Y. Objectively measured physical activity and progressive loss of lean tissue in older Japanese adults: longitudinal data from the Nakanojo study. J Am Geriatr Soc. 2013;61(11):1887-1893. doi:10.1111/jgs.12505
CrossRef - PubMed - Akune T, Muraki S, Oka H, et al. Exercise habits during middle age are associated with lower prevalence of sarcopenia: the ROAD study. Osteoporos Int. 2014;25(3):1081-1088. doi:10.1007/s00198-013-2550-z
CrossRef - PubMed - Muscariello E, Nasti G, Siervo M, et al. Dietary protein intake in sarcopenic obese older women. Clin Interv Aging. 2016;11:133-140. doi:10.2147/CIA.S96017
CrossRef - PubMed - Yang LJ, Wu GH, Yang YL, et al. Nutrition, physical exercise, and the prevalence of sarcopenia in elderly residents in nursing homes in China. Med Sci Monit. 2019;25:4390-4399. doi:10.12659/MSM.914031
CrossRef - PubMed - Efendi V, Ozalevli S, Naz I, Kilinc O. The effects of smoking on body composition, pulmonary function, physical activity and health-related quality of life among healthy women. Tuberk Toraks. 2018;66(2):101-108. doi:10.5578/tt.50724
CrossRef - PubMed - Lean MEJ, Vlachou P, Govan L, Han TS. Different associations between body composition and alcohol when assessed by exposure frequency or by quantitative estimates of consumption. J Hum Nutr Diet. 2018;31(6):747-757. doi:10.1111/jhn.12583
CrossRef - PubMed - Liedman B. Symptoms after total gastrectomy on food intake, body composition, bone metabolism, and quality of life in gastric cancer patients: is reconstruction with a reservoir worthwhile? Nutrition. 1999;15(9):677-682. doi:10.1016/s0899-9007(99)00123-9
CrossRef - PubMed - Choi MH, Kim KA, Hwang SS, Byun JY. CT-quantified muscle and fat change in patients after surgery or endoscopic resection for early gastric cancer and its impact on long-term outcomes. Medicine (Baltimore). 2018;97(52):e13878. doi:10.1097/MD.0000000000013878
CrossRef - PubMed

Volume : 18
Issue : 6
Pages : 682 - 688
DOI : 10.6002/ect.2020.0027
From the Department of Transplant Nephrology and Surgery, Nagoya Daini Red Cross Hospital, Nagoya, Japan
Acknowledgements: The authors have not received any funding or grants in support of the presented research or for the preparation of this work and have no potential declarations of interest.
Corresponding author: Hiroki Fukuhara, Department of Transplant Nephrology and Surgery, Nagoya Daini Red Cross Hospital, 2-9 Myouken-cho Nagoya City, Aichi 466-8650, Japan
Phone: +81 52 8321121
E-mail: hiroki_fukuhara@yahoo.co.jp
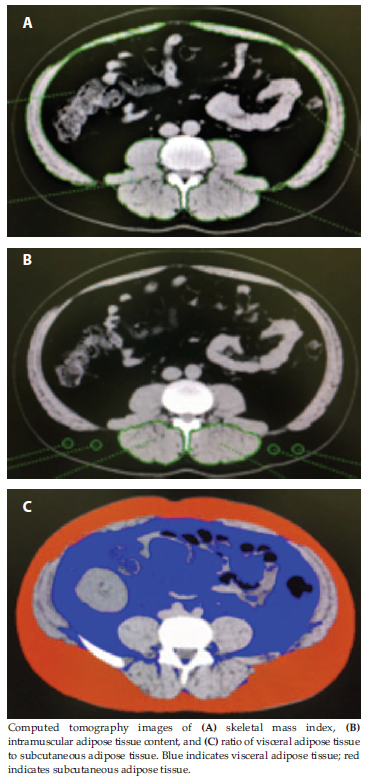
Figure 1. Body Composition Analysis With Cross-Sectional Computed Tomography Images
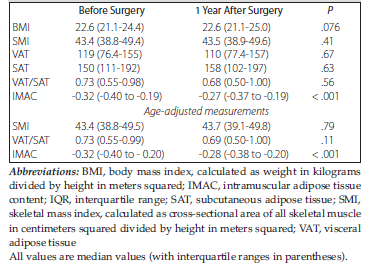
Table 1. Body Composition Analysis of Patients Before Surgery and 1 Year After Hand-Assisted Laparoscopic Living Donor Nephrectomy
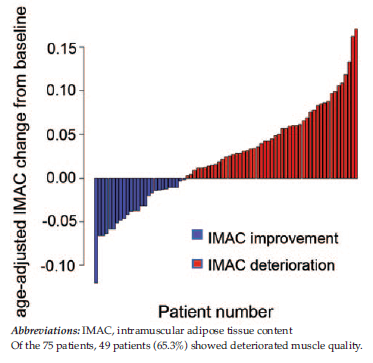
Figure 2. Age-Adjusted Intramuscular Adipose Tissue Content Change From Before Surgery to 1 Year After Surgery
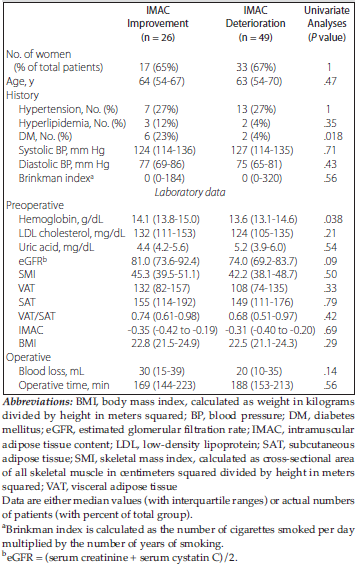
Table 2. Comparison of Preoperative Characteristics Between the Intra-muscular Adipose Tissue Content Improvement and Deterioration Groups
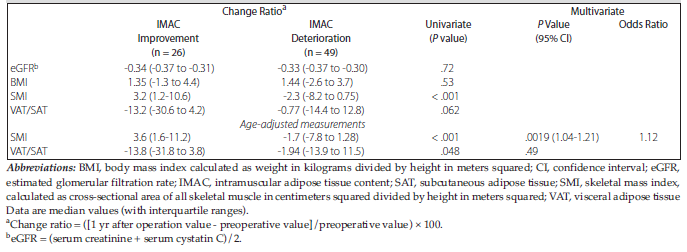
Table 3. Changes in Renal Function and Body Composition Between the Intramuscular Adipose Tissue Content Improvement and Deterioration Groups
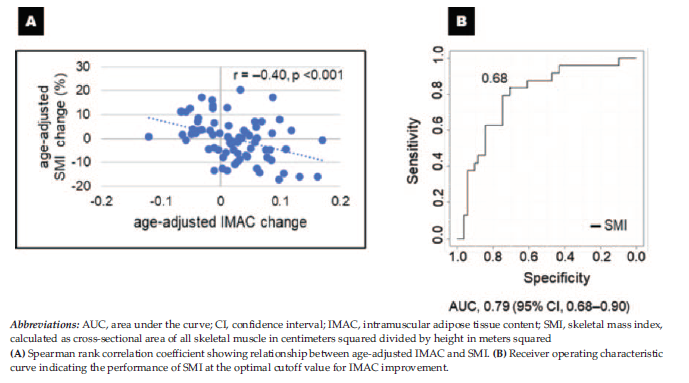
Figure 3. Relationship Between Age-Adjusted Intramuscular Adipose Tissue Content and Skeletal Mass Index and Receiver Operating Characteristic Curve